MONDAY, 25 NOVEMBER 2013
The phenomenon of pain has long been a topic of speculation and inquiry. In Greek mythology, algea were the spirits of pain and suffering, bringing body and mind to a state of grief, sorrow and distress. More recently, the British psychiatrist Ronald D. Laing encapsulated the overwhelming dominance of the sensation, stating “the only pain that can be avoided is the pain that comes from trying to avoid pain”. To this day, pain remains a leading source of morbidity and loss of productivity, and its reduction is therefore one of the liveliest sectors for academic research and drug development. At first glance, pain seems an unfortunate biological peculiarity. But could pain in fact have evolved for some useful purpose?A clue to answering this question lies in the reality of a painless life experienced by rare individuals with congenital insensitivity to pain (CIP). Although appearing normal in all other sensory and cognitive aspects, an injury that would cause agonising pain to the rest of us leaves those with CIP indifferent. As ideal as this situation may seem, it comes with a price: typically CIP severely reduces life expectancy. A lack of awareness of the tissue damage incurred by harmful stimuli means concealed injuries remain untreated, eventually causing life-threatening conditions such as widespread bacterial infections. Even when extremely cautious, people with CIP are at risk; a woman giving birth survived only because an observant physician realised she was undergoing a serious internal complication, normally diagnosed by intense pain. Other frequent characteristics are skin burns, scarred lips due to self-biting and bone fractures or joint deformities due to inappropriate limb use. Only with much effort and guidance can these people lead near-normal lives by increasing their awareness of dangerous situations and acting accordingly. It becomes evident that pain is a sophisticated protecting mechanism, allowing us to safely interact with the world around us by imposing limits on exploratory behaviours, particularly when young. Thus, upon encountering a threatening situation, pain serves to minimise physical damage; touching a hot object triggers a reflex reaction that drives your hand away, even before you are consciously aware of the danger. Moreover, pain facilitates the healing of injuries that have already occurred; a fractured leg hurts so that you become aware and take measures to assist recovery, such as immobilisation with a plaster cast.
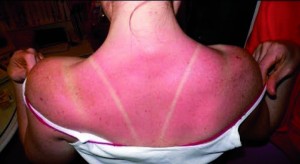
So, if pain is such a glorious adaptation, why are we so eager to get rid of it? Despite the obvious benefits of feeling pain, there are scenarios where it remains a deeply unpleasant experience with very limited usefulness. For instance, it is not helpful for a dental patient to feel pain when under the care of a qualified professional. Perhaps the best example of unwanted pain is persistent (chronic) pain which, unlike ‘normal’ (acute) pain, extends far beyond the expected period of healing. Common chronic pain symptoms are spontaneous pain as well as exaggerated responses to naturally painful or even non painful stimuli. You can get a good idea of the latter when showering after a long sunbathing session on a Mediterranean beach in summer; the sunburned skin becomes hypersensitive to warm water and this is abnormally registered as pain. Another intriguing manifestation is ‘phantom limb pain’, encountered in amputees. These patients report peculiar sensations coming from their missing limbs, such as ‘clenched fists’ and excruciating pain. Apart from nerve trauma, a plethora of diseases including diabetes, viral infections and cancer can lead to chronic pain, while more common conditions such as back pain and migraines also fall within the spectrum of chronic pain syndromes. As a result, the prevalence of chronic pain is as high as 20 per cent in Europe, representing a major cause of misery that diminishes working ability and social interactions. Unfortunately, current pain relief options such as aspirin and opioids are largely inadequate and/or associated with adverse sideeffects and addiction issues.
Early neurophysiological studies identified unique pain-encoding neurons in the peripheral nervous system, called nociceptors. These cells extend their up to one metre-long extensions to regions such as the fingertips and are remarkable in that they can encode the intensity of a stimulus; the more painful the stimulus, the more frequently these neurons send signals. All these signals are promptly transmitted to the spinal cord and subsequently relayed to the brain where pain is evaluated and an appropriate response generated.
The careful study of individuals with pain insensitivity has revealed that the trait runs in families, implying that clues to the underlying cause can be found in their genes. Strikingly, when their DNA was sequenced, a number of unique alterations in single genes was uncovered. When the same mutations were introduced into mice, they resulted in attenuated pain-sensing. In a complementary approach, other scientists examined people born with pain hypersensitivity and discovered genes associated with the extreme pain. Importantly, both methods have identified similar genes expressed in nociceptors, such as those encoding specific ion channels—membrane proteins involved in the generation of electrical signals in neurons. The pharmaceutical challenge now is to exploit this information to develop drugs that diminish chronic pain but retain the protective role of acute pain.
But do some of us feel more pain than others? The answer is yes—we can measure that, for instance by applying a temperature ramp on a subject’s hand until they call ‘ouch!’. Such experiments show that identical twins (100 per cent gene match) have more similar pain thresholds than non-identical twins (50 per cent gene match), emphasising the importance of genetic make-up. However, environmental influences can modulate the inherited gene dynamics; a fallen child who is encouraged to get up and carry on will probably develop more stoical reactions compared to one subjected to parental overreaction. The cultural setting is also instrumental; while pain thresholds are fairly similar between sexes, males tend to exhibit higher pain tolerance, in agreement with the ‘macho-man’ stereotype. In other words, although both sexes feel pain to a similar degree, males are less likely to express it. Even for a given individual, pain is finely shaped by environmental circumstances and personal expectations. Anecdotes underscoring the importance of context include reports of soldiers being completely unaware of gruesome injuries in the heat of a battle.
Brain imaging studies have been employed to try and understand how pain processing occurs, however it appears that no single pain center exists. Instead, a whole matrix of cross-talking structures is in operation. These approaches have provided additional insights, informing us for example of an elevated engagement of the limbic system in women, explaining why pain tends to elicit a greater emotional response in females.
It is perhaps reasonable to assume that motional pain, like physical pain, has evolved in umans for similar risk-aversion purposes. The ear of disastrous heartache often drives us to eigh situations more realistically and proceed with caution. But as in the case for physical pain, the danger and potential rewards can be strangely appealing. After all, we all like a little bit of chili in our food! While the conscious brain is struggling to make sense of it all, pain will continue to protect us and ensure we cherish the accomplishments for which we suffer. As the saying goes—no pain, no gain!
Christopher Tsantoulas is a postdoctoral researcher at the Department of Pharmacology